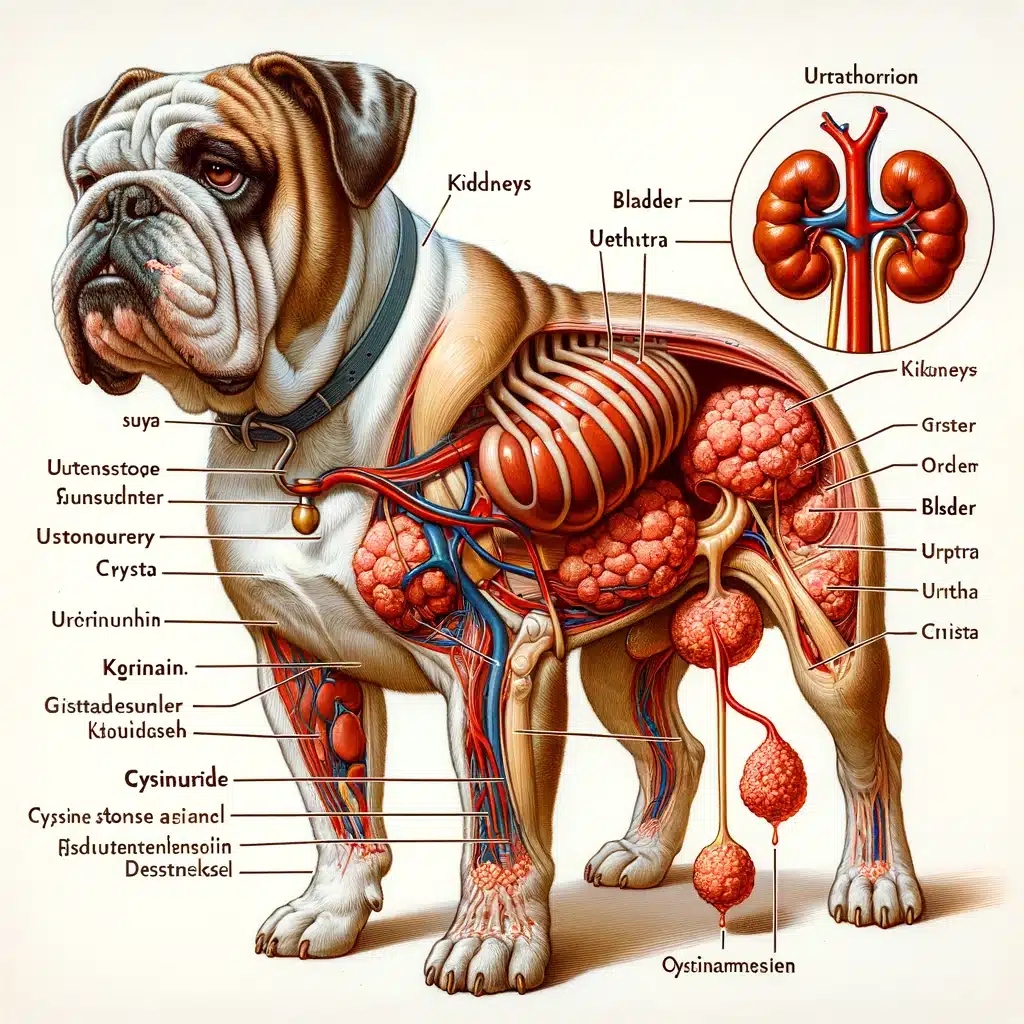
Cystinuria in dogs
Cystinuria is a serious genetic condition that primarily affects bulldogs and can lead to serious health problems. In this article, we will detail the causes, symptoms, and genetic aspects of cystinuria and provide effective management strategies for breeders and dog owners.